(Part 1)
After countless hours of research, attending seminars, and treating hundreds of individuals in my practice, I’ve come to believe that neuroinflammation is one of the most commonly overlooked problems affecting people who have experienced fluoroquinolone toxicity. “Floxed” refers to individuals who experience symptoms resulting from the use of fluoroquinolones, a class of antibiotics used to treat bacterial infections. These symptoms can range from extreme fatigue, tendon rupture, and joint and muscle pains to nerve pains and nervous system disturbances like neuroinflammation.
Neuroinflammation is inflammation of the brain, and it occurs when the brain’s immune system is activated in response to an inflammatory challenge, such as the use of fluoroquinolones. Research shows that fluoroquinolones love fat tissue, and since the human brain is primarily composed of fat, neuroinflammation can present as a variety of problems. Many people who come to me for help are in a dichotomy, meaning they have symptoms that seem opposing or unrelated.

For example, an individual may experience Achilles tendon pain accompanied by pain in their elbow. Others might report mood swings, anxiety, depression, intrusive thoughts, or simply not feeling or acting like themselves. However it manifests, it’s essential to pinpoint this neuroinflammation and address it with a proper treatment plan in order to recover. If left untreated, a tendon tear will seem like nothing compared to the neurological problems that might lie ahead.
For someone with neuroinflammation, it’s almost as if their brain is on fire. It’s important to understand that the brain doesn’t have pain receptors like other parts of the body. If you hit your thumb with a hammer, pain receptors will let you know that something is wrong by causing you to feel pain in your thumb. However, the brain doesn’t respond in the same way. If you could theoretically hit your brain with a hammer, it would not elicit that same pain response. Instead, the brain signals there’s something wrong using different methods, like brain fog, memory problems, anxiety, depression, thoughts of suicide, insomnia, reduced brain endurance, and chronic fatigue.
Chronic Fatigue and Other Symptoms of Neuroinflammation
Chronic fatigue is a common symptom of neuroinflammation that I often see in patients. It’s similar to driving your car around with the emergency brake on. The car has to work harder, requiring more energy and gas, just to complete the task it was meant for. That is your brain when it’s inflamed. It has to work ten to twenty times harder when neuroinflammation is present, which results in a spectrum of symptoms ranging from slight brain fog to full-blown chronic fatigue. In extreme cases, untreated neuroinflammation can lead to coma, seizures, difficulty speaking, and tremors.
The Subtle, Moderate, and Severe Symptoms of Neuroinflammation
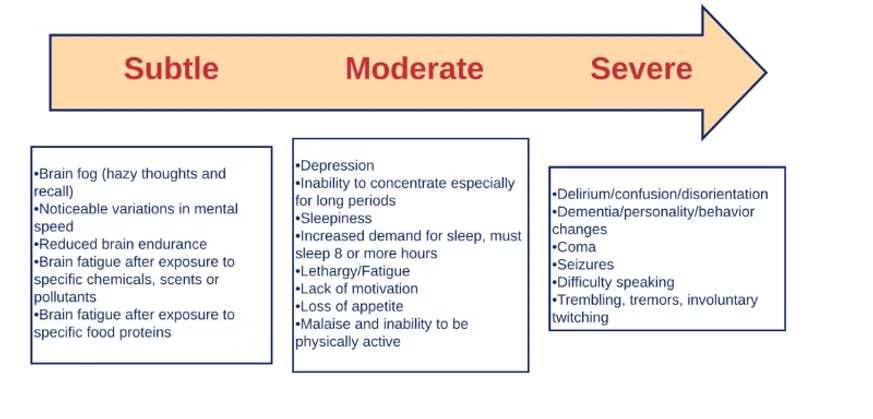
Many people have some or all of these symptoms, but it’s essential to determine which are present and how to classify them. I’ve broken down the list of possible neuroinflammation symptoms into three categories: subtle, moderate, and severe. It’s important to identify your symptoms so that they can be addressed properly with a treatment plan.
Subtle symptoms of Neuroinflammation:
Brain fog, reduced mental speed, and reduced brain endurance are classified as subtle symptoms of neuroinflammation. Experiencing brain fatigue after a long drive, where you’re being exposed to strain and stressors over a period of time, is one example. Another is experiencing brain fatigue after exposure to certain chemicals or scents, or after eating certain foods.
Moderate symptoms of Neuroinflammation:
Mental health disorders like depression and anxiety fall into this category. Inability to concentrate on tasks, excessive sleepiness, lack of motivation or appetite, insomnia, and the inability to be physically active are also moderate symptoms of neuroinflammation.
Severe symptoms of Neuroinflammation:
Difficulty speaking, tremors, disorientation, and involuntary twitching can be signs of severe neuroinflammation. Shaking, or lack of balance when completing simple tasks like walking, can also be present. More serious symptoms like seizures, dementia, and even coma are possible if left untreated.
If these symptoms sound familiar to you, then you may be suffering from neuroinflammation or brain inflammation. In the next part of this blog series, I’ll go over the different tests available to determine whether you have neuroinflammation and how severe it might be
Frequently Asked Questions (FAQ)
Fluoroquinolone toxicity refers to a collection of symptoms caused by fluoroquinolone antibiotics, which may include tendon pain, joint and muscle issues, nerve pain, fatigue, and neuroinflammation.
Neuroinflammation is inflammation of the brain triggered when the brain’s immune system is activated. It can cause symptoms like brain fog, memory problems, anxiety, depression, fatigue, and even severe neurological issues if left untreated.
Symptoms range from subtle brain fog and reduced mental speed, to moderate issues like depression, anxiety, and insomnia, to severe conditions such as tremors, seizures, difficulty speaking, or even coma.
Fluoroquinolones accumulate in fat-rich tissues like the brain. This can overstimulate the brain’s immune system, leading to inflammation that causes neurological and mental health symptoms.