Part 3
As much as I wish I could tell you there was only one cause of neuroinflammation, that is simply not the case. If you’ve been following along in this series of blogs about “brain on fire” symptoms and causes, you’ve learned that neuroinflammation can be caused by fluoroquinolones or other drugs breaking down the blood-brain barrier. However common this may be, other causes of neuroinflammation do exist and I’ll break those down for you here. It is important to know which is the cause of your specific case of neuroinflammation so that it can be addressed in a treatment plan for your recovery.
What else can cause “brain on fire” symptoms?
Some causes of neuroinflammation include head trauma, concussions, micro strokes, and stress. These causes are even more significant when you consider that the damage they do is irreversible.
The importance of barriers
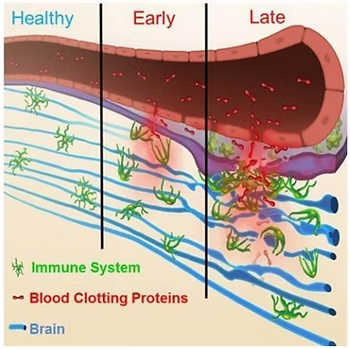
The above graphic shows a cross-section of your bloodstream. Looking at the sections marked as “Early” and “Late” in the image, you can see ruptures in the artery surrounded by blood-clotting proteins. As the figure demonstrates, the broken arteries can act like a garden hose that has been punctured. The pressure of the water inside the hose causes streams to shoot out through the punctures with some force. The same happens in your bloodstream, which can push unwanted substances through the blood-brain barrier and into your brain. The attached astrocytes along with the inflammatory process in your brain will begin to cause damage, resulting in a range of symptoms.
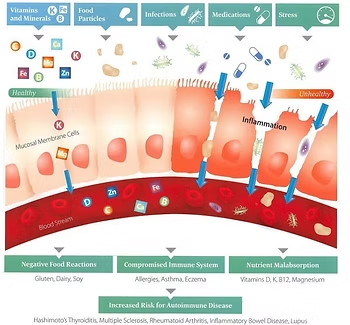
Like the blood-brain barrier, the gut also contains a one-cell-thick membrane separating the stomach contents from the bloodstream. The above graphic shows a comparison between a healthy, impermeable gut membrane (left) and an unhealthy, leaky gut (right).
Because of inflammation caused by a number of sources, the gut on the right has had its one-cell lining broken down, creating gaps large enough for a variety of unwanted material to breach into the blood. Once in the blood, these unrecognizable intruders trigger the immune system, which brings on symptoms such as negative reactions to certain foods. This inflammation can also cause malabsorption, meaning the essential nutrients in your food are not absorbed by the body.
How do you know if you’ve got a leaky gut?
For the majority of people, having two to three bowel movements per day without gas, diarrhea, bloating, or heartburn are signs of a healthy gut. Many people have leaky gut even if no gastrointestinal (GI) symptoms are present. This leaky gut allows trillions of bacteria in the intestines to leak into the bloodstream, making their way eventually to the brain through the blood-brain barrier. The end result is always inflammation.
As the blood-brain barrier begins to break down due to this leaky gut, a whole host of symptoms may appear. To make things even more frustrating, you may struggle to find someone who makes the connection between these new symptoms and GI or leaky gut issues. New research shows, though, how these issues relate, and it has to do with the vagus nerve.
What is the vagus nerve?
The vagus nerve extends from the lower intestines to the back of the human head. Research suggests that harmful bacteria from the gut can make its way to the brain through the vagus nerve, causing inflammation and other symptoms. This is why it’s essential to address gut health issues to prevent neuroinflammation.
Blog on how to strengthen your Vagus nerve
Why Doctors Don't Discuss This Connection
The link between gut health and neuroinflammation is well-established, yet many doctors don’t discuss this connection. By understanding the link between gut health and brain inflammation, you can take steps to prevent neuroinflammation and preserve your brain health.
In conclusion, identifying the cause of neuroinflammation is crucial for proper treatment and prevention of further damage. Factors such as head trauma, stress, and leaky gut syndrome can all cause neuroinflammation, highlighting the importance of addressing these issues early on. By taking steps to improve your gut health and overall wellbeing, you can protect your brain and prevent the onset of neuroinflammation.
Frequently Asked Questions (FAQ)
A leaky gut allows bacteria and toxins to pass into the bloodstream. These can then travel to the brain, either by crossing a compromised blood-brain barrier or via the vagus nerve, triggering a neuroinflammatory response.
Yes. It's possible to have a "leaky gut" without obvious digestive issues like gas or bloating. The inflammation can be systemic, with the primary symptoms manifesting as brain fog, fatigue, or mood changes instead of gastrointestinal distress.
The vagus nerve is a direct communication pathway from the gut to the brain. Harmful substances or inflammatory signals from an unhealthy gut can travel along this nerve to the brain, directly contributing to neuroinflammation.